Evidence
Animation helps to overcome barriers of health literacy
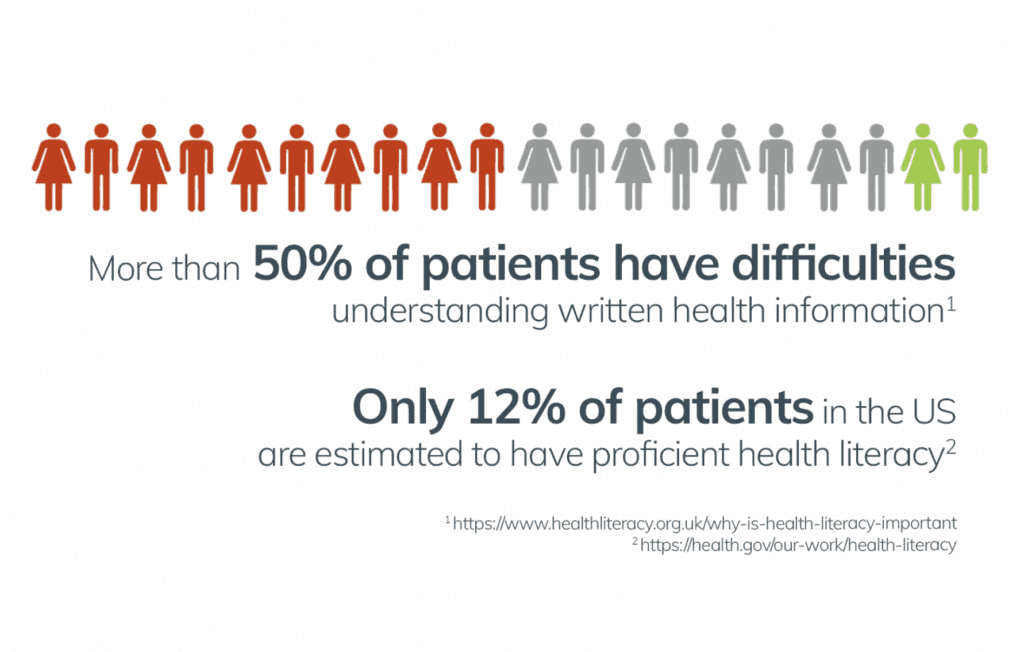
It is crucial for patients to understand health-related information to achieve best-practice care. Research, however, indicates that many find it difficult to process the complex information they receive. This exposes a need to communicate in a way that allows vital health information to be understood across literacy levels.
Research supports the use of visual formats and animations to improve patients’ ability to understand, process and act on health information. Our solutions assist healthcare professionals in educating patients through animated narratives to improve health outcomes in today’s fast track healthcare sector.

Empowered patients are stronger patients
Educating patients through visual cues and visualising what they can expect before, during and after a treatment can influence their ability to manage their health. Research suggests that improved knowledge helps to boost self-confidence and self-management skills in patients.
Empowered patients are stronger patients who will make better partners for healthcare providers in a treatment process. When patients, families and caretakers actively participate in the health outcome, it reduces time-consuming procedures for healthcare providers who meet increasing demands to reduce operational costs.
A qualitative leap and a reduced use of resources
Business cases indicate that patients who are given access to My Treatment™ place less strain on the healthcare system as opposed to patients exposed to conventional communication. This implies a qualitative leap for the patient and a reduced use of resources in the primary sector and at the individual ward.
Hospitals with My Treatment™ have found the solution to reduce the need for numerous in-person meetings. They have experienced a decrease in surgery cancellations and a reduction in the number of days that patients spend at the hospital. Hospital wards have moreover registered less incoming phone calls concerning standard information.

References
Vil du gerne vide mere?
Har du lyst til at høre mere om Visikon Analytics?
Udfyld kontaktformularen nedenfor og vi vil række ud til dig hurtigst muligt.
